Welcome to the Virtual MS Center!
Ask any question you want about Multiple Sclerosis and one of our experts will answer it as soon as possible.
|
Here is My Question:
After HSCT is it possibly to get pregnant if I am 26 years old? Answer: Stem cell transplantation (HSCT) is currently in the research phase for individuals with multiple sclerosis (to determine safety, efficacy, and long-term risks). At present, HSCT requires various levels of chemotherapy to aid in the "re-setting" of the immune system. Chemotherapy medications do have the potential to result in "sterilization" of the patient (chemotherapy in general terms affects all dividing cells in the body, including cells in the ovaries and testes). We should learn more about HSCT through current research, but at present, I cannot answer your question with complete confidence. Even with data to come in the future, exposure to conditioning regimens with various forms of chemotherapy could increase the risk of conception difficulty. Approaches to this potential problem include harvesting ova from women and sperm donations from men prior to undergoing treatment A. Scott Nielsen Neurologist and MS Specialist at Kaiser Permanente Here is My Question:
My daughter is on Tysabri for MS in Australia but she seems to have had relapse, her white blood cells are higher than they should be, will she be able to continue with this medication? Answer: Thanks for the question. Elevated white blood cells are common when using Tysabri. By virtue of how this medication works, a process of "demargination" occurs where white blood cells no longer cross the blood brain barrier and do not stick to the blood vessel wall (leading to an excess of circulating white blood cells). This is normal. Determining the effectiveness of Tysabri for a given patient is something your daughter's neurologist can help with. Some considerations for your doctor will be 1) how long has the Tyasbri been used, 2) are the symptoms indicative of a confirmed relapse (some symptoms may not be an actual relapse), and 3) what was the MS disease course prior to starting the therapy. Since I do not know your daughter's situation, I cannot comment on the usefulness of Tysabri in her case. However, I have had patients that need a little more time on the medication before the disease gets under better control. I would encourage you to attend the clinic visit with your daughter if able and discuss with the neurologist. A. Scott Nielsen MD MMSc Neurologist and MS Specialist at Kaiser Permanente Use the search box in the upper right on this page and type in "Tysabri" to learn more about Tysabri. Here is My Question:
After visiting my GP he suggested to maybe think about using Avonex. My MS is inactive but he said this would slow things down as I have nerve pain and after activity things get worse. He said this medicine works before it gets bad or active. He was talking about injections once a week. Any advice on this? Answer: Avonex, similar to the other disease modifying therapies, have been shown to do 3 main things: 1) cut down on the frequency of MS relapses, 2) cut down the number of new lesions on the MRI scans, and 3) reduce the accumulation of disability in the short term (and likely long term). Based on your question, I have reservations about the use of Avonex (or any disease modifying therapy) to help your "nerve pain" that gets worse after activity. It sounds to me that you are experiencing the fluctuating symptoms of MS that occur due to old MS scars/damage. In that case, use of symptomatic (rather then disease modifying) therapies are in order. For MS to truly be "inactive", we look for no clinical relapses, new MRI activity, or accumulated disability over time. To answer this question, it requires the expert care of an MS specialist. I would encourage you to see one of these specialists to answer your question regarding a need to use Avonex (or similar therapy) versus symptomatic management. Here is a link to help you find an MS specialist/MS team in your area http://www.healthcarejourney.com/just-been-diagnosed-with-ms.html A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center Here is My Question:
My question is this: After many tests (Alzheimer's and dementia), the neurologist has said that MS is the cause of memory problems for a 63 year old man. Many say there's no way to really diagnose the difference of whether the memory loss is due to the MS or other causes, even with doing a spinal fluid. The reason I ask this question is because when he answers questions, he answers like it is two years ago... is there way to tell if MS is really causing his memory loss? Thank you. Answer: The pattern of cognitive disturbance in MS does differ from other disease states such as Alzheimer and other dementias. As our age advances, it can be more difficult to tease them apart. The best way of doing so is to undergo neuropsychological testing. This is a comprehensive series of tests (usually paper/pencil but can also include computer tasks) that is administered in a controlled environment and interpreted by a neuropsychologist. These tests can last hours, and occasionally can be split up into consecutive days in order to minimize the effect of fatigue on the results. The neuropsychologist will compare the test-takers performance to those of similar age and background to ultimately come to an informed/educated conclusion regarding the cause of the cognitive dysfunction. These results can also help to craft a rehabilitative program (ie, for memory) that can be used to help the patient leverage their cognitive strengths to help compensate for any weaknesses. I'd recommend speaking with the neurologist about this, if not already done. A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center Question:
Hi again, I previously asked whether Aubagio was my next best option. Well, after 5 weeks and further symptoms that hasn't worked out for me either. So that's Copaxone, Rebif, Cytoxan, Tysabri, Rituxan, Plasmapheresis, monthly steroids, Copaxone again, Tecfidera & Aubagio I've tried thus far, none working for me as I continued to progress over the last 20yrs. If I were your patient, now considered Progressive-Relapsing, where would you suggest I go from here? A friend of mine is stable on Methotrexate-similarly disabled as me and has tried everything. I had marked progression on Rituxan & the 2 orals. I am in a scooter full time & as of the past year mostly unable to go anywhere but doctor's appointments. Any further progression & I will be unable to care for myself/live independently. Any advice is appreciated! (I see my MS Specialist neuro next week). Help!! Answer: I'm sorry to hear of your difficulties with the MS despite the various therapeutics you have tried. I think it is important to keep in mind that all of the disease modifying therapies (DMTs) are partially effective. Sometimes we get lucky and a patient's disease seems to go into a long-lasting remission after going on a DMT. When this happens, it may be that the DMT chosen is a near "perfect fit" for the individuals type of MS, or it was a coincidence and their MS was going to quiet down anyway. However, for many patients, we do expect to see some breakthrough disease activity, even on a good DMT. Therefore, reasonable expectations for the DMTs must be understood. I also think it is worth noting that the DMTs don't necessarily exert their full influence immediately, but can take some time (on the order of months). I would hesitate on labeling any DMT as a failure based on symptoms that started shortly after initiating the DMT. Lastly, the indication for a DMT (in my mind) is evidence of inflammatory disease activity (ie, confirmed MS relapse, new or enlarging lesions on the MRI, or contrast enhancing lesions). Unfortunately, there is no proven therapy for patients who have transitioned from the relapsing/inflammatory phase of the disease to the progressive phase. I do share your concern about progression and doing everything possible to retain as much of that as possible (with the end goal of retaining independent function). If your neurologist feels that you are still in the inflammatory phase of the disease (ie, you could still benefit from a DMT), then there is the new biologic (Lemtrada). Patients in the studies of Lemtrada who received this demonstrated an attenuated progression of disability compared to Avonex. This drug is not something to take lightly as it has a significant risk of autoimmune disorders associated with it. If your neurologist feels that you are no longer in the inflammatory phase of the disease, then a focus on rehabilitative medicine and occupation therapy to maximize functional independence is warranted (this can be used in addition to DMTs as well). I hope this helps. A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center Question:
I have 2 questions after receiving results of my yearly MRI's and my first Dexa Scan. Question #1 Is it often seen that MS patients develop pretty severe Osteoporosis? I recently had the first Dexa Scan I've done and the findings show Lumbar Spine T-Score -1.9 and 0.0838 gm/cm Bone mineral density, and Left Femoral Neck T-Score of -3.4 and 0.473 gm/cm Bone Mineral Density results showing Osteoporosis which I was given Fosamax to treat. Question #2 Are hemangioma and meningioma the same issues? Are they considered "not a concern, an incidental finding?" When would they be a concern? Is this something that neurology follows? In the MRI Cervical Spine w/without contrast they found:Enhancing Hemangioma @ T1 Vertebral Body and Broad Based Protrusion at C6-C7. In the brain MRI findings: small area of developmental venous anomaly or capillary telangiectasia. I have often been told I have a Meningioma in the R Front Lobe that is very small and appears calcified. Answer: Osteoporosis is seen in MS and may be related to several indirect causes of the disease. Bone strength and density is responsive to stress (ie, weight bearing) as well as adequate calcium intake and vitamin D. MS can lead to less physical activity (ie, less weight bearing) and spending more time indoors and out of the sunlight (resulting in deficient vitamin D). Moreover, some medications used for symptomatic treatment of MS can also lead to thinning of the bones. Simple ways to help mitigate those possible effects is to supplement with vitamin D3, calcium, and exercise (under your physician's supervision). Fosamax, as you have been treated with, can also be used in the right circumstances. Of course, there are other medical reasons for osteoporosis, and this is best investigated/treated by your primary care physician. For your second question, vertebral body hemangiomas are benign and not uncommonly seen on imaging for MS. Also, a develop venous anomaly is an incidental congenital finding. Meningiomas are most commonly benign growths of the meninges (or covering of the brain). Small meningiomas are typically asymptomatic and are monitored over time using MRI. Most of the time, nothing needs to be done about them. Your neurologist can monitor this (if it is even necessary based on your circumstances). Hope this helps. A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center
Here is My Question:
Is there a risk using contrast with getting an MRI? Answer: Typical contrast used for MRI is called gadolinium (a paramagnetic agent that comes across as bright on certain MRI sequences). This is usually fairly well tolerated, although there is a small risk for a drug reaction, and kidney injury. The kidney injury is not common, but can occur more frequently in individual with kidney impairment at the time of the gadolinium administration. Most institutions require a recent blood test (creatinine) to check kidney function prior to the MRI. It is also not recommended to receive multiple/frequent gadolinium-enhanced MRIs within a short period of time as this may increase the risk of kidney injury (or gadolinium associated nephrotoxicity). For the typical MS patient, this is not a significant concern. A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center Here is My Question:
My question requires some background information. I am a 46 year old female diagnosed in 1999 when I was 31 years old. My 1st documented symptom happened in '94. I have tried the following treatments: Copaxone '99-'04, Rebif '04-'06, Cytoxan while on Rebif in '06, Tysabri '07-'08 straight onto Rituxan in '08-'10. Just after Rituxan I had 8 weeks of Plasmapheresis followed by 2 years of monthly IVIG & Steroids only '11-'13. All of these treatments were stopped due to antibodies and/or continual progression/ineffective response. In 2013 I decided to go back to Copaxone which I stayed on until an MRI showed active lesions in April '14 (my 1st mri to show 'active' lesions in all this time). I started Tecfidera in July '14 & had further progression which prompted me to stop it in Nov '14 just as Lemtrada became approved in the US. My neurologist advised a drug holiday while waiting for Lemtrada certification. With no idea when certification may come & 5 months of no treatment I decided to try Aubagio while waiting, which I am in my 3rd week of now. I am now considered Relapsing-Progressive, am in a scooter full time, cannot take a step, stand up straight or raise my arms above my head. Since Tecfidera I am losing the use of my right hand. I believe my EDSS is 8-8 1/2. I have two questions: 1. When Lemtrada does become available to me, having had no positive result from Chemo, Tysabri or Rituxan, is its mechanism of action likely to have an effect on my particular MS case? If so do I have any hope of it stopping my progression being at the stage that I am? 2. And if not Lemtrada is Aubagio the right DMD to try at this point. Thanks for your time! Answer: I'm sorry to hear of your experience with the various DMTs. As physicians, we try out best to match up an individual patient's form of MS to the "right" DMT. However, we do not have a biomarker (ie, a blood test) that can tell us exactly where the trouble is in the immune system (for a given patient) so we could more readily match that immune dysregulation to a DMT with a specific and complimentary mechanism of action. It really is a "trial and error" process. What's more, there is the possibility that an individual with MS may have a disease course that will not be stopped or significantly altered by any of our currently available DMTs. From what little I know about your case (and this opinion cannot substitute for the opinion of your specialist who knows you), you appear to have persistent inflammatory disease activity (particularly given the new MRI activity you mention). This signals to me that there is still a chance that a DMT could be helpful in your situation. Lemtrada is the newest DMT approved for use. It is very effective (when looking at the data from the pivotal clinical trials) in reducing inflammatory disease activity. However, it does come with a significant (potential) downside--autoimmunity. Specifically, there is a greater risk of developing a condition where your immune system could start attacking your platelets (causing serious bleeding), kidneys, and thyroid. These tend to be treatable conditions, but they are not insignificant. Whenever considering a DMT, you and your physician must weigh the pros/cons. We do not expect that our DMTs will reverse already accumulated disability, but they may mitigate further progression (at least in the short term... ie, a couple years). This is something that would need to be considered in your case. These are not easy decisions, and I think it comes down to what your goals are and the level of risk you are willing to assume. I hope this helps. A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center Here is My Question:
First a little background on myself. It took me 10 years to get diagnosed. My Neurologist and I have discussed the fact that at the time of my diagnosis I may have already progressed to SPMS. I started taking Avonex, then Copaxone, tehn Tecfidera and finally Gilenya. Obviously the first three did not work out for me and I had a bad reaction to Gilenya. I also tested positive for the JC Antibodies ruling Tysabri, by my choice. Now I am not taking any DMT's. Since getting off any DMT I have noticed I have noticed a changed in my symptoms. I have become more moody and I have been having Migraines on a regular basis. I have also noticed my other symptoms have ramped up, being the pain in my legs and fatigue. So my question is as follows, is it possible that my MS is progressing as my Neurologist and I have theorized? And am I moving closer to SPMS if I am not already there? Thank you in advance for answering my question. Answer: The transition to Secondary Progressive MS (SPMS) is not a single point in time, but in the real sense of the word--a transition. Individuals can still have relapses during this transition as well. With that said, we are trying to get away from these disease subtypes/monikers because it doesn't really help us much in terms of treatment recommendations. As a field, we are trying to move to a paradigm where we ask a very simple question: Is your MS still inflammatory? The reason why this is important is that our disease modifying therapies (DMTs) are designed to reduce inflammation. While it is true that we tend to see less signs of inflammation in the classically described SPMS (and primary progressive MS), there are individuals that still demonstrate inflammatory disease activity despite their diagnostic assignment to a progressive form of MS. Inflammatory disease activity is manifest by clinical attacks (or relapses) of MS, and signs of new, enlarging, or enhancing lesions on MRI of the brain and spinal cord. In my mind, these objective findings outweigh the older MS descriptors--that are somewhat arbitrary. In order to determine if someone is inflammatory (or progressing), this should be done with the help of a neurologist who has been tracking your exam over time (preferably with objective measures such as walking speed/time, cognitive performance testing, and the neurologic exam). This is important because not all symptoms (perhaps those you are describing) are due to new or inflammatory disease activity, but is a manifestation of older MS scars that are disrupting nerve signal transmission. There are many reasons that can occur, and the neurologist can help determine if this is the case. In many instances, conservative measures can go a long way in mitigating those symptoms (that are not due to a new MS attack) to make your function in daily activities easier. I would not necessarily interpret an increase in symptoms as a sign of progression to SPMS. That determination should be done with objective data obtained by a neurologist over time. Hope this helps. A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center Question:
To my absolute horror I had bowel incontinence twice in the last week. I have suffered from IBS for many years. I am 71 and functional with no aids. Is this the beginning of a new MS symptom? Super scary. Suddenly in the middle of a walk, no control. Answer: Bowel dysfunction due to MS tends to manifest mainly as constipation, but some can also experience fecal incontinence (accidents). When a scar of MS involves the part of the nervous system that helps coordinate signaling to the bowels to evacuate (located primarily in the spinal cord--especially the lowest segment), these bowel symptoms emerge. Other contributors to bowel problems that are related to MS include: immobility or sedentary lifestyle, dehydration (ie, avoiding liquids because of bladder problems), poor dietary intake of fiber, and the acknowledgement that many different medications prescribed to treat other MS symptoms can cause bowel dysfunction as a side effect. All the more reason to review your symptoms with the MS specialist. Here is a blog I wrote that goes into further detail as well as management strategies. Hope this helps. http://www.healthcarejourney.com/q--a-for-virtual-ms-center/bowel-problems-and-ms A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center #bowelincontinence #multiplesclerosis Question:
I was diagnosed with RRMS in November, 2014 (I've had it since 2007, but being an athlete kept the MS unknown until November 2014). Since my last exacerbation in January 2015, i have been having spasticity and very strong pain in both legs and feet. I even have to use a walker. I feel very good, but my legs are bothering me a lot. (I have gone to physical therapy a few times, but it gets bad again). Why does this happen? Is spasticity a normal symptom of MS? I also would like to know how does vitamin helps MS? I drink 100,000mg a week of vitamin D (prescribed by my doctor). Will I ever be able to do my exercises again?. Thank You!!!! Answer: In the upper right hand corner of this page (and of every page on the website) you will find a search box. If you type in the topic you are interested in (such as spasticity, vitamins) you will find a wealth of information and many answers to similar questions asked by people with MS. Spasticity is a common symptom of MS, and many things and several things will aggravate spasticity, acting as a “trigger” for spasms. These include:
In your case, I would start with reviewing our pages on spasticity http://www.healthcarejourney.com/spasticityspasmscramps.html which discusses ways to manage it, as well as all the various blogs that have been posted about spasticity http://www.healthcarejourney.com/apps/search?q=spasticity. Then I suggest you make sure that the physical therapist you are seeing has experience with multiple sclerosis. Here is a blog describing the benefits of having a physical therapist who specializes in MS and how to find one http://www.healthcarejourney.com/physical-therapy-blog/does-physicaloccupational-therapy-help-with-symptoms-from-ms Working with a physical therapist who specializes in MS will maximize the likelihood of resuming your exercise routine. In terms of vitamins, you can read all our blogs about vitamins here http://www.healthcarejourney.com/apps/search?q=vitamins A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center Question:
Here is my family history:
When other methods proved ineffective about 4 years ago, I began Tysabri infusions. It has seemingly stopped MS in its tracks. No new visible lesions on yearly MRI's and no new symptoms since beginning Tysabri. When reading the results of the study (as best I could understand), the fact that my mother has Alzheimer's, and her sister and and I both have MS, is not a coincidence and highly suggests a genetic factor on the maternal side of the family? What I fear is that I may have passed a gene on to my 14 year old daughter. Are there any tests or avenues available for early detection of any of the disorders which seem to be related to MS or the like? I attribute my early detection of the disease, and aggressive therapy choices, for minimizing the damaging effects of MS (and I'm sure my more "lucky" genes than those of my neighbor or classmates which have progressive MS). Is there any thing I can do to help protect my daughter, other than making her aware of how critical it is to be cognizant of her body and be very mindful of any changes that may appear to be out of the norm? Any advice/knowledge you could share would certainly be appreciated. I am part of the TOUCH progam which I believe is an ongoing study group through Tysabri which tracks and shares my progress. Is there anything else I could to add and give aide to this large database being created? Answer: Thank you for this thoughtful question. MS certainly has a genetic component to its development and manifestation; however, it isn't a simple genetic pattern, but more complex. There are over 100 "susceptibility" genes that have been identified that are associated with MS. In nearly every instance, these genes are part of the immune system. The "susceptibility" moniker emphasizes that just because an individual has genes associated with the disease, that doesn't mean they will go on to develop MS. In fact, there is evidence that a first degree relative of someone with MS will have a 4% lifetime risk to develop the disease themselves. We suspect that individuals with a certain genetic "load" of these susceptibility genes in addition to a yet to be determined environmental factor(s) triggers the MS disease process. So, genetics is a piece of the puzzle, but not the whole puzzle. Please see the blog on this subject by Dr. Greenberg and Dr. Kinkel: READ MORE If interested, you and your daughter may be eligible to participate in a genetics/epidemiological study on this subject through Brigham and Women's Hospital in Boston, MA: READ MORE A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center Question:
After years of clear MRI's and good neurological exams, why should I keep taking the DMT? I have been through Copaxone, Avonex, Tysabri and now Tecfidera. Would it be unwise to take maybe a month, six months or a year off from everything and come back to treatment if things change? Answer: This is a good question, but not one that I cannot reasonably answer over a blog. (Mainly because I do not know your full story and I haven't had the opportunity to review your scans or examine you in person.) What I can do is speak on DMT-governing principles which you can take back to your physician for discussion. Some guiding principles in the use and prescribing of DMTs:
In your specific case, I have no way of knowing if you've met the criteria of "disease free" status. Cycling through different DMTs usually means that your physician has found something that suggests that your prior DMTs haven't been effective enough. I would suggest you speak with your physician about this. I hope this helps. A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Center #MS #diseasemodifyingtherapies #multiplesclerosis #DMTs Here is My Question: After 2 years on Tysabri my neurologist suggested that I start getting infusions each 6 weeks instead of each 4 weeks, even though I am JCV negative. What would be the benefit? What is the evidence about efficacy of 6 week or 8 week dosing regimen? Thanks! Answer: Good question. The main reason such a change in dosing frequency (from every 4 weeks to every 6 or 8 weeks) is considered is based on preliminary evidence that doing so may reduce the risk of progressive multifocal leukoencephalopthy (PML) while maintaining the effectiveness of Tysabri. The rationale behind this is that we know that Tysabri saturates alpha-4-beta-1 integrin receptor by >80% after the infusion, and the saturation remains above 75% when you go back to get your next infusion 4 weeks later. At 6-8 weeks after the infusion, the saturation drops to ~70% and then ~40% two weeks later. The interaction between this receptor on your white blood cells and the blood vessel wall allows the cell to get into the central nervous system and potentially lead to an MS relapse. Tysabri blocks this interaction which is presumably why it works so well in reducing the number of clinical attacks, MRI lesions, and attenuating disability over time. This receptor-Tysabri interaction is a double-edged sword, however. The white blood cells are also needed to survey the central nervous system and eradicate foreign invaders (ie, the JC-virus that causes PML). So, by altering the dosing frequency of tysabri, we are hoping to allow enough saturation of the integrin receptor by tysabri to protect patients from MS but at the same time, allow enough opportunity for the white blood cells to gain access to the nervous system to "keep an eye" on foreign viruses--particularly the one that causes PML. Preliminary data on this topic presented at the American Academy of Neurology meeting in 2014 can be found below:
This multicenter observational data is preliminary but so far suggests that extending the dosing of Tysabri to every 6 to 8 weeks appears to maintain the drug's effectiveness against MS and at the same time, they have not observed a case of PML. Of course, this is just preliminary, and they are continuing the observational study to confirm these findings.
Hope this helps. A. Scott Nielsen MD MMSc Virginia Mason Multiple Sclerosis Clinic Here is My Question:
I want to start by saying that I know I am very blessed to be dealing with the relatively minor issues that I do. I've done a little research, trying to learn a little about MS so I wouldn't have to ask silly questions, but it seems the more I read the less I felt like I really knew about the topic. I am a 55 year old male and was diagnosed with primary progressive MS about 3 years ago. Symptoms like leg and torso numbness, burning pain in leg and torso, spasticity, fatigue, and pain associated with unrelated back issues as well as some cognitive and bladder issues have been gradually getting worse. The burning in my leg is pretty much constant now and too intense to tolerate at times, and the other symptoms have worsened also making walking much more difficult and range very limited. And sleeping... My understanding is that my treatment options are limited to treating each symptom, and it seems to me at least that to this point that has had limited success. So anyway, the question I guess is really one of expectations. I just need to know...are the gradually worsening symptoms what I should be expecting and something I just need to deal with somehow? Is there any point to whining to my neurologist again? Answer: I'm sorry to hear about your struggles with the progressive nature of your MS. It is telling that you refer to your problems as "relatively minor issues." I applaud you on your ability to take perspective and notice where things are good in respect to your MS and functional status. Some individuals (regardless of whether they have MS) always focus on the negatives, which in my experience as a physician working with patients dealing with a chronic illness, is very disabling by that fact alone. You are correct in that the current state of MS therapeutics is extremely limited for reparative strategies due to the underlying damage to the nervous system caused by MS. There are some interesting experimental therapeutics currently being investigated in phase I and II clinical trials right now (anti-lingo and rhIgM22 antibodies), and we patiently wait on what we learn about these biologics. You are also correct that the progressive phase of MS is primarily dealt with in terms of treating symptoms. Based on the nature of the symptoms, strategies involving symptomatic pharmaceuticals, cognitive rehabilitation, and physical medicine and rehabilitation measures can be used (among others). I would counsel you to always bring up your symptoms and concerns with your neurologist. While it is important to recognize the limitations to medicine and the state of treatment for MS as it currently stands (which it appears you do), it is important to keep in mind that there are symptomatic therapeutic approaches that could be very beneficial to you. As a MS neurologist, I must admit that I can't read my patient's mind, and I find it very difficult to know how to help unless they speak up. We genuinely want to help, and you shouldn't feel that you are whining (your word). Please see this communication from a patient perspective on this topic: http://www.healthcarejourney.com/patient-blog/communication. Many times, the physiatrist (a doctor who focuses of rehabilitation medicine) will play a lead role in the progressive symptomatic treatment of patients with MS in concert with the neurologist. Most comprehensive MS centers have these physician subspecialists that can be integral in your treatment team. Hope this helps, A. Scott Nielsen, MD MMSc Virgina Mason Multiple Sclerosis Clinic 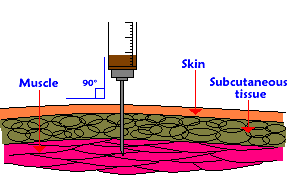 I will answer this question under the assumption that the "journey" asked about is regarding a disease modifying therapy (DMT) called interferon-beta 1a (also known as Avonex). This DMT is injected into the muscle once weekly and was approved by the FDA for the treatment of relapsing multiple sclerosis. Once injected (about 1 milliliter) into the muscle, absorption of the drug occurs and reaches the blood circulation which delivers it throughout the body. The active ingredient is a Type I interferon (which is identical to interferon made in our bodies as a response to a viral infection). The interferon is simply a string of protein building blocks (or amino acids) that also has a sugar chain attached to it. This complex (protein and sugar) interacts with receptors on various cells in our body (think of a lock and key relationship where the interferon is the key and the receptors are the locks). When the interferon unlocks the receptor on the surface of different cell types, it causes various chemical reactions inside the cell. One of these reactions includes the movement of a protein complex into the nucleus of our cells (this is the part of the cell that houses our DNA--or genetic code). This protein complex attaches itself to part of the machinery of the cell nucleus that expresses our DNA. (This machinery is like a Xerox copy machine of sorts. It recognizes specific genes and can literally copy the genes or translate the genetic code into other proteins that can leave the nucleus and do work that needs to be done throughout our body.) In the case of interferon, the machinery induces the expression of genes to fight viruses, provide anti-proliferative signals, and "modulate" the immune system. It is the induction of these "modulatory" genes that presumably exert the beneficial effects in MS patients (ultimately reducing the bad inflammation in the brain and spinal cord, the number of MS attacks, new scars on the MRI scans, and reduce the accumulation of physical disability over time). Clinical trial evidence suggests that the intramuscular (IM) route of administration was superior to intravenous (IV) but comparable to subcutaneous (just under the skin) in the sense that IM and subcutaneous injection reached a peak of biological effect at 48 hours rather than 24 hours by the IV route). Also the overall exposure (what we term the "area under the curve" when we plot blood levels of biological response markers over time after the injection) to the interferon was greatest using the IM route compared to IV or subcutaneous injections. Interferon is metabolized (ie, digested) by the liver as many drugs are, and eliminated from the body primarily through our kidneys. The half-life (the time it takes to half the amount of drug in the blood stream) is approximately 19 hours. A. Scott Nielsen MD MMSC Virgina Mason Multiple Sclerosis Center Here is My Question:
Can someone who was diagnosed with MS by both monthly evoked response tests and a lumbar puncture (but before there were M.R.I.'s), but has a negative M.R.I. now, can they still have the disease? Answer: By monthly evoked response tests, I assume you are referring to visual evoked response (VER) and somatosensory evoked potential (SSEP). Since the advent of MRI, we use the VER and SSEP less frequently. VER measures the function of your visual system and SSEP (how we use them) tend to measure the ability of your spinal cord to transmit electrical signals. If there are delays in these tests, it indicates that there may be an MS lesion or scar within those pathways. The lumbar puncture (LP) looks for signs of chronic inflammation that is specific for the nervous system (and tends to be positive in 90 to 95% of MS patients). With that said, it is possible to make a diagnosis of MS based on these tests (or your story and neurologic exam alone) without the use of MRI. However, it is a red flag in my mind to make a diagnosis of MS with a completely normal MRI of the brain. There are mimicking diseases of MS that can render a normal MRI scan of the brain but show disease in the optic nerves and spinal cord. If there is any question, getting another independent opinion from an MS specialist is reasonable. Hope this helps. -A. Scott Nielsen, MD Virginia Mason MS Center Here is My Question:
I have been taking Ditropan for bladder problems for several years until fairly recently at a dose of 5mg 1 to 2 times per day. Relapses in the past few months have meant that I now take 5mg 3 times per day, with limited positive results. However, I have very recently been told that Ditropan's effect is very limited if it is taken with food, and that it should be taken either 1 hour prior to, or 2 hours after food. The comment was also made that as a dry mouth is a common side effect, "if you don't have a dry mouth, it's probably not working very effectively." I am quite annoyed at not being told this, and have checked the drug information sheet provided by the pharmacy, which makes no mention of taking it on an empty stomach. Is this true? Also, I have found elsewhere that one of the contra-indications to taking this is having a hiatus hernia, which I have. This has never been discussed with me by my neurologist, gastroenterologist or general practitioner. So what should I do? Answer: It sounds like your MS has been active recently and has influenced the complex micturition reflex (you can read more about this reflex in Dr. Kinkel’s blog here: http://www.healthcarejourney.com/urinationbowel-problems.html). Ditropan treats overactive bladder (detrusor) function. However, there is more to the story than the detrusor for micturition. I’d suggest discussing this with your neurologist and a separate urological consultation may be needed to address the recent changes in your bladder function (ie, 1- to identify any other factors at play, and 2- develop a treatment strategy specific to your current bladder needs). Keep in mind that sometimes higher doses of Ditropan may be needed (up to 30mg/day)—although I do not recommend doing this on your own, but with the close observation of your treating physician (if it makes sense to do so in your specific situation). To answer your specific questions about Ditropan:
Hope this helps. -A. Scott Nielson, MD, MMSc, Virginia Mason |
PLEASE NOTE: This information/opinions on this site should be used as an information source only. This information does not create any patient-HCP relationship, and should not be used as a substitute for professional diagnosis and treatment. Please consult your health care provider before making any healthcare decisions or for guidance about a specific medical condition.
Archives
March 2024
Categories
All
|
||||||||